1. 引言
原发性干燥综合征(pSS)是一种主要累及全身外分泌腺的慢性自身免疫性疾病,以唾液腺和泪腺的症状为主,是在遗传、病毒感染和性激素异常等多种因素共同作用下,导致机体细胞免疫和体液免疫的异常反应,通过各种细胞因子和炎症介质造成组织损伤,可同时累及甲状腺、肺脏、肝脏、肾脏等多种器官出现多种临床表现,严重危害人类健康。sCR2是C3a片段的终末产物C3d、C3dg的细胞受体,也是B细胞上的EB病毒受体[1] ,是一种单链表面糖蛋白[2] 。sCR2具有抑制补体经典途径和旁路途径的活化,协助清除体内的免疫复合物,调节B细胞功能的作用。因此,sCR2可以对抗过度的炎症和免疫反应。近年来大量研究表明CR2在自身免疫病的发展过程中起作用。sCR2在原发性干燥综合征患者血清中的变化及其意义,目前国内尚无相关报道。本研究用ELISA法检测了30例原发性干燥综合征患者及20例健康体检者血清中sCR2的浓度,探讨原发性干燥综合征患者血清中sCR2的变化及意义,为了解pSS的发病机制提供新的理论试验基础。
2. 材料与方法
2.1. 一般材料
30例原发性干燥综合征患者(观察组),均为2011年1月至2012年10月在大连大学附属中山医院风湿免疫科住院病人。全部为女性,平均年龄为(46.1 ± 13.2)岁。所有患者均符合美国风湿病协会(ARA)2002年修订的SS的诊断标准。对照组20例均为健康体检者,男3例、女17例,平均年龄为(32.4 ± 9.4)岁。两组性别、年龄差异无显著性(P > 0.05),具有可比性。
2.2. 观察指标及方法
2.2.1. 观察指标
所有患者及正常对照均于清晨空腹时采静脉血,以所测的血清sCR2浓度为观察指标。
2.2.2. 方法
以固相的双抗体夹心酶联免疫吸附实验法(ELISA)为本实验研究方法。
2.3. 仪器及试剂
2.3.1. 仪器
酶标仪,移液器等。
2.3.2. 试剂
购自美国RapidBio Lab公司生产的sCR2 ELISA试剂盒。
2.4. 检测方法
将抽取的所有患者及正常对照的3毫升静脉血,离心后取血清放入血清管中,−80℃冰箱冻存。试验前先将试剂盒及冻存的血清标本平衡至室温。从sCR2试剂盒中,取出已包被抗体的酶标板,每孔加入20 μL sCR2标准品和血清,每孔加入100 μL抗人sCR2抗体工作液,室温30 min甩干液体后洗涤5次;每孔加入150 μL抗人sCR2 POD,室温温育30 min后洗涤5次;每孔依次加入100 μL TMB显色液,室温温育20 min;每孔依次加50 μL Stop Solution终止液,450 nm波长酶标仪测OD值,计算浓度。应该还要加HRP标记的抗体才能与底物结合;
2.5. 材料分析
以OD值为纵坐标,sCR2的标准品浓度为横坐标,做出标准曲线(已知两者之间为多项式关系),见图1。根据多项式方程及各样本的OD值得出sCR2的浓度。
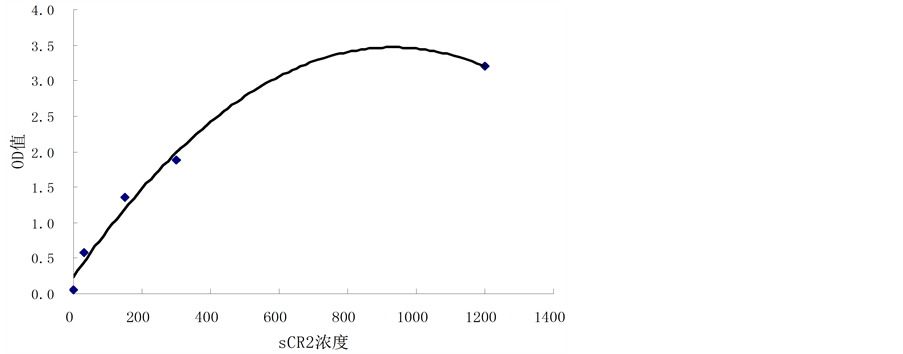
Figure 1. Chart of sCR2 concentration curve
图1. sCR2浓度曲线示意图
2.6. 统计学方法
所得数据以均数 ± 标准差(x ± s)表示,采用SPSS17.0统计软件统计,统计方法采用方差分析,两组间比较行独立T检验。检验水准α = 0.05。sCR2水平与pSS患者其他实验室指标之间关系分析采用直线相关分析,并计算Pearson相关系数r,以P < 0.05为差异有统计学意义。
3. 结果
1) 两组血清sCR2水平,观察组SS患者血清sCR2水平为(75.78 ± 62.09) ng/ml,对照组为(314.45 ± 272.09) ng/ml。由表1可以看出,观察组均明显低于对照组,P均<0.05。1,抗SSA和/或抗SSB抗体阳性组,血清sCR2水平明显低于阴性对照组(P < 0.05,表2)。
2) 将SS患者血清sCR2水平与SS患者血清中RF及C3的浓度进行相关分析,发现SS患者血清sCR2水平与其RF (r = −0.292 P = 0.118 (P > 0.05))及C3 (r = −0.209 P = 0.267 (P > 0.05))无相关性;将SS患者血清sCR2水平与SS患者血清中免疫球蛋白IgG浓度进行相关分析,发现SS患者血清sCR2水平与免疫球蛋白IgG及血沉存在明显正相关(r = −0.829 P = 0.000 (P < 0.05); r = −0.549 P = 0.002 (P < 0.05))(分别见下图2、3)
4. 讨论
补体受体2型(complement receptor 2, CR2,又称CD21)是补体激活调节剂(regulator of complement activation, RCA)家族的一员,是C3a片段的终末产物C3d、C3dg的细胞受体,也是B细胞上的EB病毒受体[1] ,是一相对分子质量为145,000单链表面糖蛋白[2] 。主要分布于所有成熟B细胞和滤泡树突状细胞上,也存在于某些上皮细胞和T细胞系的原始细胞[3] 。CR2有两种形式,一种是膜相CR2,一种是可溶的CR2 (soluble complement receptor 2, sCR2)。后者只具有膜相CR2胞外的活性部位,可与膜相CR2竞争配体[4] 。原发性干燥综合症(primary Sjogren’s syndrome, pSS)是主要累及唾液和泪腺的自身免疫疾病。B淋巴细胞高反应性成为其最突出的免疫学特征之一,临床上可以看到多数pSS患者体内存在着高免疫球蛋白血症[5] 。除了血清免疫球蛋白的增高,大约60%~70%的患者的抗核苷酸抗体和类风湿因子高滴度和高红细胞沉降率。T淋巴细胞对B淋巴细胞的调控失常是B淋巴细胞高度活化产生自身抗体导致自身免疫病的重要因素之一[6] 。在T辅助细胞的作用下,B淋巴细胞功能异常,产生多种自身抗体、多克隆的免疫球蛋白以及免疫复合物,致使唾液腺和泪腺等组织发生炎症和破坏性病变[7] 。

Table 1. The sCR2 concentration of the comparison results between the observation group and the control group
表1. 观察组与对照组之间sCR2浓度的比较结果

Table 2. The comparison results between sCR2 concentration of anti SSA/SSB antibody positive group and negative control group
表2. 抗SSA和/或抗SSB抗体阳性组与阴性对照组之间sCR2浓度的比较结果
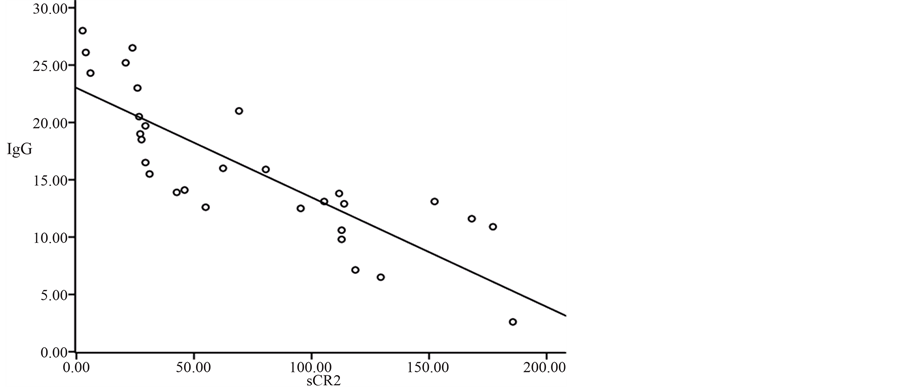
Figure 2. Schematic diagram of the correlation between immunoglobulin IgG level and serum sCR2 level in pSS patients
图2. pSS患者血清sCR2水平与免疫球蛋白IgG的相关性示意图
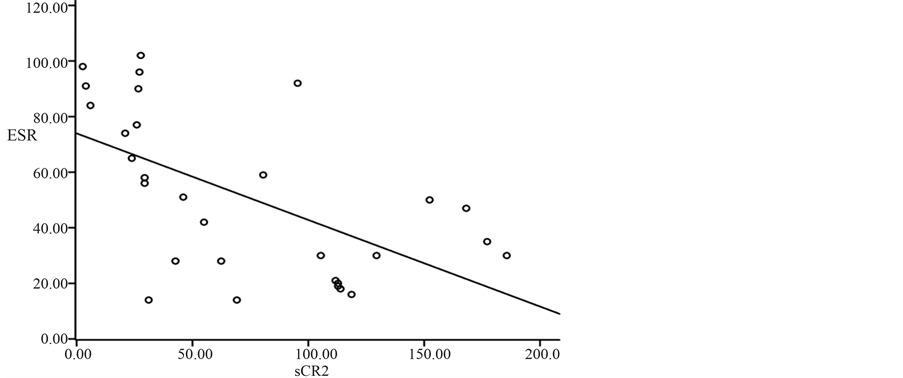
Figure 3. Schematic diagram of the correlation between ESR level and serum sCR2 level in pSS patients
图3. pSS患者血清sCR2水平与血沉的相关性示意图
本研究中我们发现,SS患者血清sCR2水平明显低于正常对照组,在SS患者中,sCR2与年龄和性别无关。由此本实验得出结论血清sCR2的减少与疾病本身有关,不仅会导致sCR2的低水平,而且排除了不同年龄组及性别之间的差异。B细胞受体和被免疫复合物吞噬的C3d激活B细胞从而减少了B细胞表面的CR2的浓度[5] 。因此,德国Konstanz大学的Masilamani M博士推测血清中sCR2水平的减少是由两方面引起:B细胞的激活;通过循环免疫复合物吞噬的C3d来增加血浆sCR2的清除[6] 。同时,sCR2的减少导致它的协助清除体内免疫复合物,调节B细胞功能的作用的减弱,从而加速了自身免疫病的发展,可见sCR2在自身免疫病的发生发展中起了重要作用。sCR2可与膜型CR2竞争配体,从而阻断抗原与膜型CR2结合,对抗过度的炎症和免疫反应,避免机体受到损害[8] 。曾有动物实验研究表明重组sCR2既保留了CR的功能与活性结构,也能在较低的浓度下发挥有效作用[9] 。提示sCR2在自身免疫病的临床治疗中可能发挥积极作用。本研究还发现,血清sCR2水平在pSS中与RF无关,与C3无关,但与免疫球蛋白IgG及血沉存在明显正相关,特别是自身抗体阳性组血清sCR2水平显著低于阴性对照组。表明sCR2在pSS患者体内是促进B细胞增殖的,并在调节免疫球蛋白的产生过程中起重要作用[10] 。由于sCR2水平的降低,致使B淋巴细胞反应性增高,多克隆B淋巴细胞激活使体内产生大量器官特异性及非特异性自身抗体并可出现高免疫球蛋白血症,更加剧了自身免疫反应及腺体内外损伤,提示sCR2可能参与PSS的发病过程。
5. 结论
本实验通过检测SS患者血清可溶性补体受体2(sCR2)浓度,发现其明显低于正常对照组,且与免疫球蛋白IgG及血沉存在明显负相关,提示sCR2可能参与pSS的发病过程。同时也提示我们,sCR2可能在以自身免疫性疾病的发病过程中起重要作用,为我们今后深入研究提供了新的方向。
致 谢
在此,衷心感谢王晓非教授、张永利教授、侯云华教授及实验室老师为本实验及论文提供的指导和帮助,对给予转载和引用权的资料、图片、文献、研究思想和设想的所有者,以及免疫学研究的编辑部老师表示感谢。感谢所有为本实验及论文倾注心血的人们!

NOTES
*通讯作者。